Lesson 4 - Understanding The RCM Cycle
(Revenue Cycle Management) RCM Cycle:
Revenue Cycle Management (RCM) is the core administrative and financial process that supports the entire patient care journey within a healthcare organization from initial appointment scheduling and insurance verification to medical coding, claim submission, payment posting, and final reporting. Every department involved in medical billing & coding, including front desk, eligibility verification, coding, billing, accounts receivable (AR) follow-up, and payment posting, operates within this RCM framework. A thorough understanding of RCM is crucial for all medical billing professionals to ensure accurate, timely, and compliant revenue collection.
Short Definition:
In short, the RCM cycle represents the entire medical billing and coding field processes from start to finish.
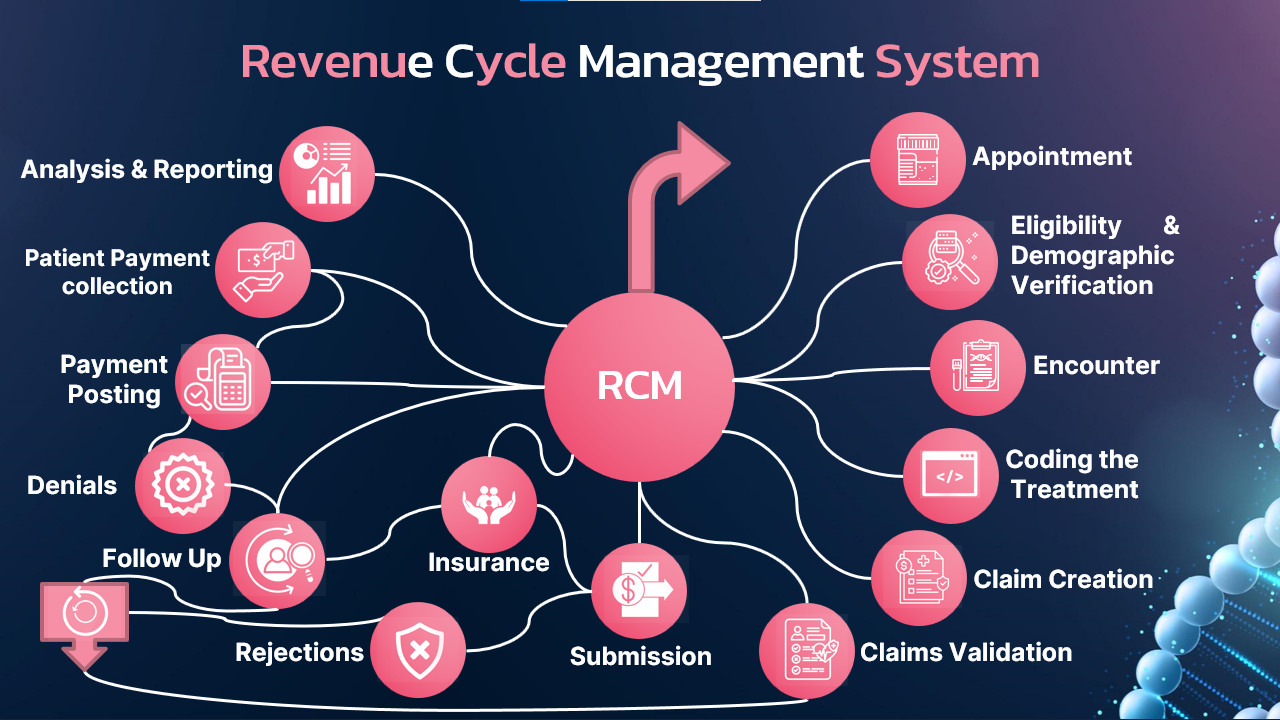
RCM Chart
 ✕
✕
Here is the step by step breakdown of the RCM Cycle:
-
Appointment Scheduling
The first step in the RCM cycle begins when a patient schedules an appointment. During this process, the front desk or clinical staff collects essential demographic and insurance information, including:
- Full name
- Date of birth
- Address
- Insurance details
Note: While appointments are usually scheduled in advance, healthcare providers also accommodate walk-in or emergency visits.
Eligibility and Demographic Verification
Once the appointment is booked, the patient's information is sent to the billing team. The billers verify the patient's insurance coverage (eligibility) and ensure that all demographic data is accurate. This step is critical for reducing claim denials due to incorrect or outdated information.
Patient Encounter
On the day of the visit, the patient is seen by the provider. During this encounter, the provider:
- Evaluates the patient
- Diagnoses the condition
- Recommends medical care, tests, or treatments
This clinical interaction is the foundation for the subsequent coding and billing processes.
Medical Coding
After the consultation, the provider’s notes and treatment details are forwarded to the medical coding team. The coders translate the medical services and diagnoses into standardized codes:
- ICD (International Classification of Diseases) – for diagnoses
- CPT (Current Procedural Terminology) – for procedures/services
Accurate coding ensures proper claim processing and reimbursement.
Claim Creation
Once coding is complete, the billing team prepares the insurance claim. This document includes:
- Patient’s personal and insurance details
- Date of service
- ICD and CPT codes
- Provider and Facility information
- Any additional payer-specific information
The goal is to create a clean, accurate claim ready for submission.
Claim Validation
Before submission, senior billers perform a thorough verification of the claim. They check for:
- Coding accuracy
- Demographic consistency
- Insurance eligibility
- Payer-specific requirements
This step reduces the likelihood of denials and rejections.
Claim Submission
After validation, the claim is submitted electronically through a clearinghouse to the insurance payer. This step may result in:
-
Rejections:
Formatting or billing errors detected by the clearinghouse must be corrected and resubmitted.
-
Denials:
Claims not meeting payer guidelines must be investigated, corrected, and resubmitted by the AR team.
Insurance Follow-up (AR Follow-up)
After submission, the Accounts Receivable (AR) team follows up with the insurance company to:
- Call insurance representatives
- Resolve outstanding issues
- Ensure timely reimbursement
Proactive follow-up plays a vital role in cash flow management.
Payment Posting
Once the insurance processes the claim, they issue:
- EOB (Explanation of Benefits)
- ERA (Electronic Remittance Advice)
Payments are posted into the practice management (PM) software, and denied services are reviewed and resubmitted if eligible.
Patient Responsibility & Payment Collection
After insurance payment, the remaining balance may include:
- Co-payments
- Deductibles
- Non-covered services
Patient statements are issued, payments collected, and posted in the PM software.
Reporting & Analysis
Billers generate monthly financial reports that include:
- Collections performance
- Claim denial rates
- Days in AR
- Payment trends
These insights help providers make informed business and operational decisions.
Conclusion
The RCM cycle is a comprehensive and multi-step process that requires accuracy, coordination, and consistent follow-up. By managing each phase effectively—from patient registration to final reporting—healthcare practices can improve cash flow, reduce errors, and enhance overall efficiency.
Note:You have read many things like clearing house, claims, deductibles, ERA, EOB, etc. like terms, we will discuss all of them in depth so don't worry and keep learning.
Do you have any question or concern?
Feel free to ask any questions related to medical billing, lessons, or our services. We will be pleased to provide you with accurate and timely responses. If you would like to share feedback or learn more about our offerings, please fill out the form below and leave us a message.
